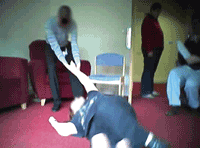
Nearly half of Castlebeck services are failing to meet essential standards of quality and safety, a report by the Care Quality Commission has revealed.
The regulator found poor governance, staff with disrespectful attitudes and patients routinely deprived of their liberty.
As a result, the CQC is taking enforcement action against four of the provider’s services: Arden Vale near Coventry, Rose Villa in Bristol, Croxton Lodge in Leicestershire, and Cedar Vale in Nottingham. It is not yet clear whether this will involve closures or fines.
The CQC, which inspected 23 of Castlebeck’s services, has concerns about a further seven.
The CQC said there were company-wide problems. These included:
● Lack of training for staff.
● Inadequate staffing levels.
● Poor care planning.
● Not involving people in decisions about their own care.
● Failures to notify the regulator about safeguarding concerns.
Lee Reed, chief executive of Castlebeck said action to rectify the problems was being taken “as a matter of urgency”. “There is no place within our organisation for services that fail to deliver high quality care,” he said.
The round of inspections was triggered by the exposure last month of alleged abuse at Winterbourne View, the Bristol learning disability hospital.
Poor governance and culture
The CQC found that the governance of Castlebeck was inadequate. Senior management had failed to put in place systems to hear feedback on service quality and then take action.
In addition, there was no clear system for communicating decisions to improve quality at senior management level down to those running services.
The CQC also said there was a lack of “visible and tangible leadership” in many services because registered managers were moved around the company, often without the CQC being told.
It said: “Many of the issues identified contribute to what we believe is a poor culture within the organisation.”
Breaching the law
The regulator found that Castlebeck was routinely breaking the provisions of the Mental Capacity Act deprivation of liberty safeguards.
The report said: “There was a restrictive practice of routinely locking bedroom and other doors within independent hospitals without a clear and specific rationale for doing this.”
It also said the sue of restraint was “common practice” but with “little or no evidence that this was used as a last resort”.
It also found that staff had received no training in understanding the Mental Capacity Act.
Ed Mitchell, Community Care legal columnist and editor of Social Care Law Today, said: “If you are regularly locking incapacitated people in their bedroom it’s almost inevitable that you are depriving people of their liberty. If you are doing that without the proper legal safeguards you are probably breaching the Mental Capacity Act.”
Kept in hospital too long
The regulator said there was little evidence staff were working to help patients towards living in the community in a reasonable timeframe.
Earlier this month Community Care found that one-fifth of patients in learning disability hospitals had been there five years or longer.
The CQC found that understaffing was responsible for a lack of one-to-one rehabilitation activities in some facilities. It also emerged that staff regularly worked 12-hour shifts, often without a break.
Referring to the report as a whole Reed said: “These concerns were identified as issues in need of addressing when I took over as Chief Executive in January this year, since when they have been the subject of internal reviews and recommendations. Action has been taken as a result that will bring about positive change for all the people in our care.”
Related articles


 Bournemouth, Christchurch and Poole
Bournemouth, Christchurch and Poole  Hampshire County Council
Hampshire County Council  Lincolnshire County Council
Lincolnshire County Council  Norfolk County Council
Norfolk County Council  Northamptonshire Children’s Trust
Northamptonshire Children’s Trust  South Gloucestershire Council
South Gloucestershire Council  Wiltshire Council
Wiltshire Council  Wokingham Borough Council
Wokingham Borough Council  Children and young people with SEND are ‘valued and prioritised’ in Wiltshire, find inspectors
Children and young people with SEND are ‘valued and prioritised’ in Wiltshire, find inspectors  How specialist refugee teams benefit young people and social workers
How specialist refugee teams benefit young people and social workers  Podcast: returning to social work after becoming a first-time parent
Podcast: returning to social work after becoming a first-time parent  Podcast: would you work for an inadequate-rated service?
Podcast: would you work for an inadequate-rated service?  Family help: one local authority’s experience of the model
Family help: one local authority’s experience of the model  Workforce Insights – showcasing a selection of the sector’s top recruiters
Workforce Insights – showcasing a selection of the sector’s top recruiters 

 Facebook
Facebook X
X LinkedIn
LinkedIn Instagram
Instagram
Comments are closed.