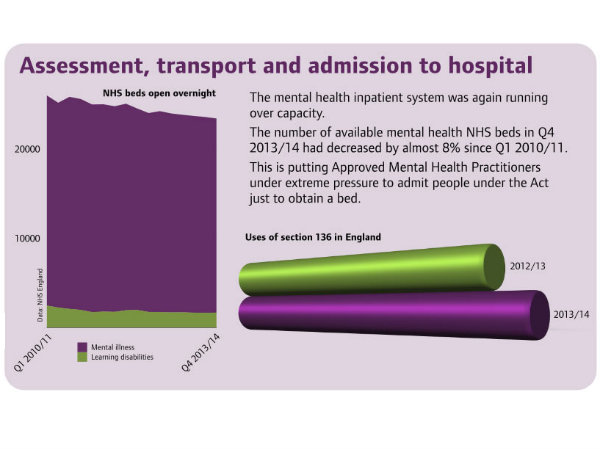
Approved Mental Health Professionals are being put under ‘extreme pressure’ by a lack of available beds to admit people in crisis to, the Care Quality Commission has warned.
AMHPs are the group of mostly, but not exclusively, social workers that carry out Mental Health Act assessments. The CQC’s fifth annual report on the Mental Health Act found that the inpatient system was “again running over capacity” in 2013-14 and the number of available psychiatric beds dropped 8% between January 2010 and March 2014.
Inspection teams saw an increase in the number of patients being sent to out-of-area hospitals and the CQC warned that the pressure on beds could also be leading to more patients being detained under the Act as professionals are left without a less restrictive option. The regulator pointed to an example where a patient might have been prepared to accept voluntary admission to a local bed, but was detained under the Act because the only option bed available was at an out-of-area hospital.
At the end of 2013-14 there were 23,531 people subject to the Act, an increase of 6% from the previous year.
“This [pressure on beds] is putting Approved Mental Health Professionals (AMHPs) under extreme pressure, and may lead to the Act being used just to obtain a bed. While it would not be lawful to use detention powers solely as a means to secure access to hospital treatment, AMHPs may be forced to choose this as the least worst option available,” the report said.
Lack of alternatives
The regulator said local areas must support AMHPs to “report, record and understand how to escalate their concerns when they have difficulties in accessing a bed” and this information should be reviewed by senior leads and raised with commissioners.
A series of investigations by Community Care and BBC News over the past 18 months have highlighted the impact of the bed shortage on staff and patients. At least eight deaths have been linked to problems accessing beds over the past two years and use of out-of-area placements has surged with patients being sent over 200 miles away for care. Both The College of Social Work and the British Association of Social Workers have raised repeated concerns over bed pressures.
This week the Royal College of Psychiatrist launched a commission to review mental health bed provision. The commission is currently seeking feedback from professionals and patients and will take evidence until March 18.
The impact of deprivation of liberty ruling
The CQC report also examined the early impact that a landmark Supreme Court ruling on deprivation of liberty in care has had on use of the Mental Health Act. The court ruling, known as the ‘Cheshire West’ ruling, effectively lowered the threshold for what constitutes deprivation of liberty in care. In doing so, it broadened the group of people in care homes, hospitals (including mental health wards) and other settings that are likely to require any deprivation of their liberty to be authorised under a legal framework.
Where a patient is in hospital to receive treatment for a mental disorder and lacks the capacity to consent to their care then, in principle, there are some cases where either a Deprivation of Liberty Safeguards (Dols) authorisation or detention under the Mental Health Act are options. Professionals must decide which legal framework is the most appropriate. Relevant factors include whether the person is objecting to the care arrangements or not.
The CQC found that in the five months since the Supreme Court ruling, 893 were detained in hospital under the Mental Health Act – an 8% rise from the previous year. The regulator warned that this was not “conclusive evidence” of the effect of the Supreme Court ruling, particularly as Mental Health Act detentions have shown a general trend of rising for years, but it said some staff and local NHS trusts had reported “a resulting increase in the number of MHA assessments carried out” in the wake of the judgement.
Other issues
Other issues raised by the report included:
- Patients are not being given information about their rights: 16% of the care records examined by the CQC did not state that staff had given information about their legal rights. This was an improvement on the previous year, where 29% of the records did not include this information but the regulator said more needed to be done.
- Concerns over advocacy provision: Only around a third of wards visited by inspection teams did provide patients with access about independent mental health advocates. And only 14% of local authorities that responded to the CQC’s survey could confirm that they had assessed the need for independent advocacy in their area.
Dr Paul Lelliot, the CQC’s deputy chief inspector for hospitals, said that the report findings should be a “wake up call” for commissioners and managers of services.
“We expect to see improvements,” he said. “We have already used these findings to improve our inspection model for services that use the MHA and to strengthen the Code of Practice so that people affected by the Act can receive better care.”


 Bournemouth, Christchurch and Poole
Bournemouth, Christchurch and Poole  Hampshire County Council
Hampshire County Council  Lincolnshire County Council
Lincolnshire County Council  Norfolk County Council
Norfolk County Council  Northamptonshire Children’s Trust
Northamptonshire Children’s Trust  South Gloucestershire Council
South Gloucestershire Council  Wiltshire Council
Wiltshire Council  Wokingham Borough Council
Wokingham Borough Council  Children and young people with SEND are ‘valued and prioritised’ in Wiltshire, find inspectors
Children and young people with SEND are ‘valued and prioritised’ in Wiltshire, find inspectors  How specialist refugee teams benefit young people and social workers
How specialist refugee teams benefit young people and social workers  Podcast: returning to social work after becoming a first-time parent
Podcast: returning to social work after becoming a first-time parent  Podcast: would you work for an inadequate-rated service?
Podcast: would you work for an inadequate-rated service?  Family help: one local authority’s experience of the model
Family help: one local authority’s experience of the model  Workforce Insights – showcasing a selection of the sector’s top recruiters
Workforce Insights – showcasing a selection of the sector’s top recruiters 

 Facebook
Facebook X
X LinkedIn
LinkedIn Instagram
Instagram
Comments are closed.