Joan has early onset dementia. She has always lived independently, but some concerns started to be raised that Joan was no longer managing so well. She had stopped going out, and her house had become cluttered and unclean.
Joan’s landlord wanted to evict her and Zoey, a senior social worker in Hampshire Adults’ Health and Care, began working with her.
It appeared that Joan had care and support needs, but she was reluctant to have a social worker involved and Zoey was finding it hard to get in contact.
But through an initiative Hampshire launched just over a year ago, called the Enhanced Support Project, Joan got access to support that helped Zoey gain her trust and work in a strengths-based way to help Joan turn her life around.
The Enhanced Support Project (ESP) was set up for people who struggle to engage with services, and where safeguarding risks relating to self-neglect are increasing without the person receiving the support they need.
Learning from a Safeguarding Adults Review led to the service being developed as “a better way to engage with people who could be forgotten because of non-engagement,” says Donna Harrison, head of service for learning disabilities, contact centre and MASH adult social care.
The Enhanced Support Project (ESP) workers are able to work intensively to build rapport and put plans in place that limit risk by involving the community and using least restrictive options and strengths-based approaches.
Specialist providers
This development has improved social work practice across Hampshire in partnership with two specialist providers – Richmond Fellowship and Home Group.
Referrals into the project are first of all measured against risk criteria. “These include signs of self-neglect, hoarding, difficulty engaging with services or a history of not engaging, and evidence that risks are escalating,” says Zoey, who has worked on the project since its launch.
This information is passed on to Richmond Fellowship or Home Group so they can start providing intensive and focused work to build relationships with individuals and identify their support needs. Once open, cases are then reviewed every two weeks to make sure continued needs and risks are properly understood and the right level of support is in place.
“Individuals needing this degree of support tend to have challenges linked to physical or mental health, substance misuse or domestic violence,” says Zoey.
Underpinning the entire project is a person-centred and trauma-informed approach that includes making sure the views and wishes of people being supported are as well-understood as possible and are clearly shared at every meeting.
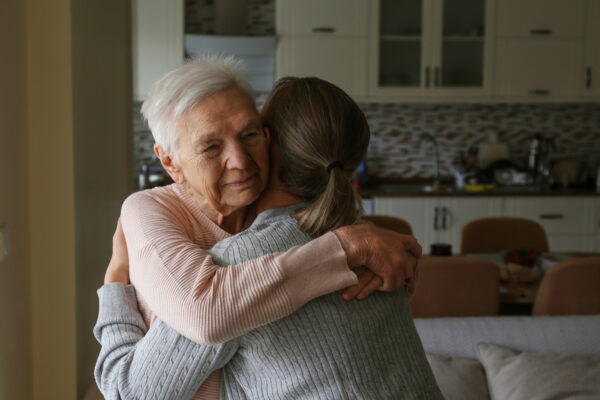
Individuals needing support may have physical and mental health challenges. Photo: Evrymmnt/AdobeStock
Community involvement
Hampshire County Council works closely with colleagues from specialist health teams and primary care services like GPs, as well as fire services, housing associations and environmental health to build up a tailored picture for each person being supported by the ESP.
Taking a multi-agency approach under section 42 of the Care Act 2014 or the multi-agency risk management (MARM) framework means that where there are complex scenarios, for example, involving substance dependency or families, other key agencies such as education, children’s services or the NHS can be ready to step in and offer support.
Risk plans can also involve support from the local community. Donna gives an example of a risk mitigation plan for John, a man who is currently street homeless. Hampshire Adults’ Health and Care has been able to establish a robust risk plan for John with local shop owners, street pastors and town rangers to offer outreach support, ensuring that his basic needs are met.
This includes shop owners keeping an eye out for him and having a contact to report any concerns, including if they have not seen him in his usual areas or if he has not been into the shop for a few days.
“This approach has been a really good example of the community working together and with John to achieve the outcomes he wants,” says Donna.
The impact of the approach Hampshire Adults’ Health and Care take, using the ESP and multi-agency, strengths-based practice, is seen in improved outcomes for people. “Getting direct feedback from people with experiences of these services is really important to us,” says Donna.
One example is an email recently received from Tanya, who had been supported by the ESP.
“Since being under the care of this amazing initiative, I have managed to claw my way back somewhat from the brink and am now beginning to see the hope for regaining my life and purpose,” Tanya says. “This has not been without setbacks but luckily, every time a new challenge presents itself, the team is there to guide me through…[It is a] truly lifesaving endeavour”.
Balancing risk and human rights
But this project is not without its challenges.
Practitioners are constantly having to tread the fine line between minimising risk to an individual and upholding their human rights to ensure that these are protected.
It can be tricky because some of the people who are supported own their own property and are not obliged to engage or co-operate with adults’ health and care, says Zoey, who has been with Hampshire for 25 years, eight of which have been in the MASH team.
But having a “clear and evidence-based” focus in risk assessments is key, she adds.
Practitioners use Hampshire’s risk assessment and escalation framework, which has been developed to support practitioners and safe decision-making around risk. The risk assessment tool supports discussion and records individual risks for a person and what is in place to mitigate them.
An escalation framework ensures practitioners are supported with shared decision making for complex risks, drawing on relevant expertise as needed within the council and from partner agencies.
“We are clear on what the harms and the potential harms are and accepting how people may want to choose to live,” says Zoey. “But [we are also] making sure we are opening up opportunities for individuals and engaging with all the right agencies as best as we can”.
For the most complex risks, practitioners can seek guidance from a risk panel. This includes heads of service and assistant directors, who can provide escalation routes to other services, such as legal, health and police, if required.
Training

Hampshire has developed internal training around hoarding and self-neglect. Photo: ronstik/ AdobeStock
Hampshire has developed internal training around hoarding and self-neglect. There is also strengths-based practice training and the sharing of best practice between teams, explains Gillian Williams, the service manager for the Contact, Assessment and Resolution Centre (CART) & MASH.
“And we do a lot of work with our case workers and senior case workers about understanding what strengths-based approaches need to look like because it’s not always around commissioned services – it’s about what that person wants and how we work with that person,” she adds.
Practitioners are also supported by hoarding forums, which are led by some of the local district councils’ own housing providers and are an opportunity to stay informed and share best practice examples.
Through the ESP, Hampshire has successfully engaged with about 75% of the 170 cases it has been involved in in the past year.
Joan, the lady Zoey is supporting, is one of them. The team has been able to involve Joan’s GP, and a community nurse visits regularly to carry out blood tests and check-ups.
Joan also has been given assistive technology, such a pendant, and has agreed to have her hedges removed from the front, which means she can open her front door.
“It’s just trying to work at the person’s pace to gain their trust and engagement,” says Zoey.
“It’s positive breakthroughs like this that make the work rewarding,” adds Donna.
If you are interested in opportunities at Hampshire County Council, check out the latest vacancies.




 Facebook
Facebook X
X LinkedIn
LinkedIn Instagram
Instagram