Story updated 28 April
There have been over 4,000 deaths involving Covid-19 in care homes England in the past two weeks – over four times the number recorded in residential and nursing homes up to that point.
The news came as health secretary Matt Hancock announced that deaths of all people who have tested positive for Covid-19 – care homes, the community, as well as hospitals – will be reported in the daily figures put out by government.
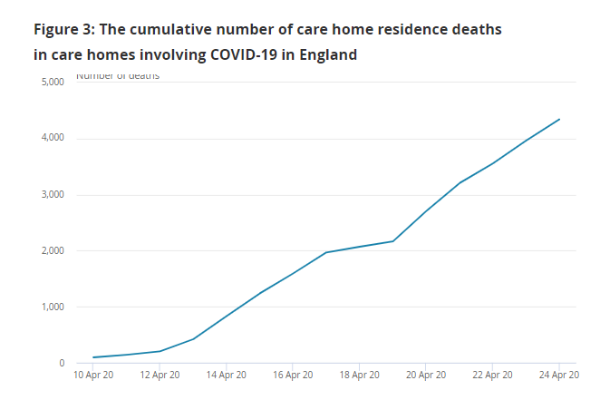
From 10-24 April, the Care Quality Commission recorded 4,343 deaths involving the disease in homes, based on notifications by providers, figures published by the Office for National Statistics released today showed.
This marks a substantial acceleration in deaths in homes from the disease. Up to 10 April, when the CQC started recording these figures, the ONS had recorded 975 deaths involving Covid-19 in English care homes.
And today’s figures show that the death rate in homes has increased during the time the CQC has been recording the figures, with 1,968 reported in the first week (up to 17 April) and 2,375 in the second. While these figures cover people dying in care homes, the CQC recorded 461 deaths of care home residents at an unknown location during this period, which may in many cases involve residents who had been taken to hospital with Covid-19 and died there.
Non-coronavirus deaths continue to dominate
However, deaths recorded as unrelated to Covid-19 in care homes have continued to mount and predominate among the total reported.
The ONS recorded 7,316 deaths in England and Wales (7,012 in England alone) in care homes in the week ending 17 April, an almost threefold increase on the total recorded in the week ending 27 March.
Of these, 4,986 (68% of the total) were not recorded as relating to Covid-19. While this is a lower proportion than the previous week, the number of non-coronavirus related deaths rose by over a fifth (21.5%) compared with the week ending 10 April.
It is possible that some of these deaths may have been incorrectly recorded as not relating to Covid-19 – for instance, if the person died with the virus but was never tested for it – but they may also reflect the consequences of overwhelming pressures on the health and social care systems.
Separate figures published by the ONS showed how far deaths in care homes have outstripped numbers in previous years. The average for the equivalent week in 2015-19 was 2,154, meaning this year’s figure was 3.4 times as high.
The ONS figures also showed a significant and rising numbers of deaths at home, with 4,570 in the week ending 17 April (416 relating to Covid-19) up 64% from 2,786 in the week ending 27 March.
The latest figures are double the average for deaths in homes for the previous five years for the equivalent week (2,344).
‘Whatever it takes’ approach needed
Responding to the rising death toll, Vic Rayner, executive director at not-for-profit providers’ association the National Care Forum, said: “The numbers revealed today make it more important than ever that we build a ‘ring of steel’ around care homes. They need the right PPE equipment, medical monitoring devices, rapid and comprehensive testing, proper funding and intensive research to safeguard the people they care for.
“This virus is not going away – this data shows that the ‘whatever it takes’ mantra must be applied urgently to protect the most vulnerable in social care, as we have to the NHS. We need action and we need it now.”
Sarah Scobie, deputy director of research at health think-tank the Nuffield Trust, said: “It is now increasingly clear that Covid-19 has gripped the social care sector tightly. The number of care home deaths are over 5000 higher than we would see in an average week for this time of year. This week, which includes deaths registered in the week ending 17th April, we have seen the number of deaths in care homes jump by 50% from the previous week.
This will have taken an extraordinary emotional and physical toll on hard-pressed care staff looking after residents.
Related articles
Hancock was challenged repeatedly by journalists at today’s Downing Street briefing on the government’s record on supporting care homes through the pandemic, including in relation to the mounting death toll and inadequate access to personal protective equipment (PPE).
In response, he said: “Care homes have been a top priority right from the start. We put out our first guidance to care homes in February and we’ve been working with them throughout.
“It’s been a focus from the start. We’ve strengthened the rules around what happens in care homes and improved infection control, and also making testing available throughout the care sector, I think, is incredibly important as we’ve ramped up the availability of testing.
“We’ve kept a close eye on this and I’m very glad that we’re now able to publish these daily data which will keep up the focus on what’s going on in care homes.”
Greater access to testing and higher PPE standards
Alongside Hancock’s announcement on recording deaths, he also unveiled an extension in testing within care homes – part of the government’s drive to ramp up testing to 100,000 a week by the end of the week, up from 43,563 yesterday.
From now on, care home residents and staff who are asymptomatic for Covid-19 will have access to tests. Previously, it was only available to staff and residents who were symptomatic, as well as residents discharged into care homes from hospital, regardless of their symptoms.
Frontline social care staff in all other settings – including social workers – will also have access to tests, under the extended access arrangements announced today.
Separately, Public Health England has produced strengthened standards for personal protective equipment for care home and home care staff.
From now on, staff will be expected to wear a fluid-resistant surgical mask, disposable gloves and apron when delivering personal care to anyone – regardless of whether they are displaying symptoms – or within two metres of anyone in the setting with a cough.
This strengthens previous recommendations, which said that social care staff should wear PPE when delivering care to someone with possible or confirmed Covid-19.
Death recording differences
There are some differences between the way the ONS and the CQC collect data. The ONS figures are based on registered deaths, where Covid-19 was noted on the death certificate, whereas the CQC ones are derived from notifications made by providers reporting that a person’s death involved the disease.
It is possible that some deaths reported by providers may not be based on a diagnosis, and may not end up being registered as involving Covid-19.
The CQC figures are dated by the time that the provider notified the regulator, whereas the ONS deaths are based on the date of death. The regulator’s figures are also likely to be provided more quickly as providers must notify the CQC of deaths without delay and they are typically provided within two to three days, while it takes, on average, four days for a death to be registered and thus recorded in the ONS figures.
The ONS and CQC figures include people without a positive test for Covid-19; however, the daily figures that the government will publish from care homes and the community, as well as hospital, from tomorrow will only include those of people who have had a positive test.


 Family help: one local authority’s experience of the model
Family help: one local authority’s experience of the model  ‘I spent the first three months listening’: how supportive leadership can transform children’s services
‘I spent the first three months listening’: how supportive leadership can transform children’s services  How senior leaders in one authority maintain a culture of excellence
How senior leaders in one authority maintain a culture of excellence  How staff support ensures fantastic outcomes for children and families
How staff support ensures fantastic outcomes for children and families  Workforce Insights – showcasing a selection of the sector’s top recruiters
Workforce Insights – showcasing a selection of the sector’s top recruiters 

 Facebook
Facebook X
X LinkedIn
LinkedIn Instagram
Instagram
In UK do we have a higher proportion of care homes than say Spain and Italy?
In the care home I work we lost 7 clients with only 1 having covid19 on death certificate. Our team is convinced that 3 more at least should of had it on theirs. Is it true deaths from covid should have cremations because some of ours didnt.